Leveraging 5G For Robotic Telesurgery
- Maria Inês Marreiros

- Apr 2, 2023
- 11 min read
The world we live in is mobile. Mobile networks have become increasingly popular in recent years, with each generation (G for short) bringing amazing breakthroughs that have shaped the evolution of humankind and technology itself. However, the advancement of cellular networks has taken almost four decades from 1G to 2G, 3G, 4G and 5G (with 6G already under development) (Ahmed Solyman & Yahya, 2022). Since 1979, each new generation has changed the way we communicate and greatly improved our daily lives. Earlier generations of mobile network technology focused on customer needs, including voice and messaging services with 2G, web browsing with 3G, and faster data and video streaming with 4G. Nonetheless, the shift from 4G to 5G has revolutionized technology. Up to 100 times faster than 4G, 5G has ushered in a new era of mobile internet, driving leaps in wireless network coverage, data transmission capacity and speed, aiming to support both customers and businesses (Haverans, 2021). With the advent of 5G, ultra-fast broadband (one of the fastest Internet connections available) became a reality, with information transmission speed and coverage reaching an all-time high level. Additionally, latency, or the time between transmitting and receiving information, dropped to a record-low level (Attar et al., 2022; Ericsson, 2018).
"5G will start a technology revolution. It will bring new power to all Information and communication technologies (ICT) and trigger sweeping changes in business. There will be new opportunities the likes of which we've never seen.” Ken Hu, Huawei Rotating Chairman

5G is about connecting everything and everyone, everywhere. The Internet of Things (IoT), or the network of physical objects (things) in which sensors, software and other technologies are embedded to connect and exchange data with other devices via the Internet, has become a reality (Ahmed Solyman & Yahya, 2022; Madakam et al., 2015). Millions of connected devices can now gather and exchange data in real-time, leading to a hyper-connected world where the physical and digital worlds converge, revolutionizing the way societies and businesses work (Hatton, 2023). 5G thus offers the opportunity for innovations such as E-health, automated manufacturing, self-driving automobiles and interconnected vehicles and transportation systems, massive video downloads, and remote control with haptic feedback, that is capable of transmitting tactile information (Attar et al., 2022). Medicine, along with telecommunications, has experienced one of the sharpest technological advancements in recent years. With the arrival of 5G, their pathways have converged and connected in unprecedented ways, improving people's health and well-being (Castro e Melo & Faria Araújo, 2020; Datta, 2021).
Real-time Patient Health Monitoring
While steam power spurred manufacturing innovation during the First Industrial Revolution, electricity fueled the Second Industrial Revolution, catapulting industrial productivity to unprecedented levels. The Third Industrial Revolution, also known as the (first) digital revolution, brought us the processing power of computers and unprecedented access to information via the internet. This has completely shaped the way we shop, consume, work and spend our free time. The modern trigger for ushering in a Fourth Industrial Revolution, or the New Digital Revolution is 5G technology (Datta, 2021; The Digital Advantage: What Is the Future of Business?, 2019). 5G will transform all industries, and healthcare is no exception. As one of the sectors most vulnerable to technological advances, the healthcare industry is being impacted by digitization, the process of converting information into a digital (i.e. computer-readable) format (Castro e Melo & Faria Araújo, 2020; Schwab, 2017). The global COVID-19 pandemic has created an urgent need for innovative approaches that enable remote care while ensuring healthcare systems are adaptable and responsive.

Telemedicine, or remote medicine, is becoming commonplace due to the higher speeds and increased reliability of 5G, enabling a maximum number of people to access healthcare. Initial screening evaluations, routine assessments, therapy/rehabilitation sessions, and increasingly visual diagnostics (namely dermatological conditions) are now conducted via two-way HD video between the patient and a healthcare provider (Haleem et al., 2021; How COVID-19 Is Changing Digital Health – and What It Means for Telcos, n.d.). This is critical, for example, for patients who cannot to travel to meet with healthcare professionals, while reducing patient exposure to infectious agents; a major concern during the global COVID-19 pandemic. One of the most thrilling future prospects of remote healthcare is the ability for anyone to check their health quickly, easily, and regularly from anywhere. The ability to remotely track patient symptoms via sensors, wearables (health tracking biosensors placed on the body to assist in the surveillance of the wearer's health data) and e-health applications has paved the way for this (Hardman et al., 2021; Liu & Ma, 2022; Yang et al., 2022). Remarkably, more than 60% of customers worldwide are willing to adopt wearables for health management, such as miniaturized blood glucose implantable sensors, wireless blood pressure sensors or networked scales (Ericsson, 2017). A notable example is the BioSticker, the first FDA-approved single-use medical device that provides continuous vital sign monitoring for 30 days. The on-body sensor continuously monitors patients' vital signs - including heart and respiratory rates and body temperature - and allows physicians to obtain data from patients in real-time (NS Medical Staff, 2020). This cutting-edge technology lays the ground for scalable remote treatment, which is critical for healthcare providers to take preventative and corrective measures to avert potential health complications (Mauricio, 2022).
Another application of 5G in healthcare is prescription compliance monitoring, an important concern in the healthcare sector, particularly for some elderly or mentally ill patients who forget whether or when they took their prescribed medications. The use of video-enabled medication adherence, which connects trained doctors and caregivers directly to the patient via video can help overcome this challenge, by ensuring the proper medication and dose are taken at the appropriate schedule (Haleem et al., 2021; Walker et al., 2019; Xushenglan, 2021). 5G is also a game changer in emergency care. Paramedics can now better treat patients in ambulances before they arrive at the hospital than was previously possible. Doctors can get a better picture of the nature of the emergency because a camera mounted on the ambulance sends high-definition video with near-zero latency between the ambulance and the hospital. The doctor can then remotely instruct the paramedic and analyze the patient's health status and symptoms to prescribe urgent treatments, which paramedics must administer on the way to the hospital (Whelan, 2022).

New Immersive Realities are Game-Changers in Healthcare
The healthcare ecosystem uses digital reality technologies such as augmented reality (AR) and virtual reality (VR) for a variety of purposes, including the detection and treatment of dementia, depression, post-traumatic stress disorders, phobias, and other physical conditions and pathologies (Mousavi, 2023). Despite their parallels, both technologies diverge in that VR is based on a computer-generated simulation that recreates a new reality, whereas AR is defined by the ability to layer digital information onto real-world elements (Makhataeva & Varol, 2020). Using devices with a video camera incorporated into their interface, AR maintains the real world at the center but enhances it with other digital details, adding new layers of perception to hence enhance reality (Augmented Reality vs Virtual Reality, 2022; Makhataeva & Varol, 2020). Mixed Reality (MR) is a novel digital holographic image technology that combines real and digital elements. Using the most advanced sensing and imaging technologies, the user can engage with and move elements and surroundings, both real and virtual (Hu et al., 2019). However, network limitations can have a significant impact on their performance. The expanded capabilities that 5G networks offer can help mitigate these limitations.
VR and AR have the potential to improve the patient experience. Immersion and engagement are critical to effective treatment; unfortunately, this is often disregarded as, when it comes to questions of life and death, patient experience is not the first factor to consider. These can be used to help patients and their families communicate better. Moreover, long-term patients can use VR to explore digital pleasant environments "outside" the hospital in the hopes of enhancing their mood and reducing anxiety or despair (Mousavi, 2023). The immersion component also opens the door to new forms of rehabilitation. An immersive virtual reality environment, for instance, can be used to alleviate pain and enhance sleep patterns. In addition, VR may be utilized to assist amputees adapt to their new condition, and patients can use a VR headset to visually overlay their lost limb to relieve phantom limb discomfort (which is the sense of pain or discomfort in a limb that is no longer present) (Mousavi, 2023; Vodovatova, 2023). Besides improving patients' experience, AR has also the potential to improve disease detection, prevention and treatment. AR systems use a combination of laser scanners and processing units. The system scans the patient's body layers and detects veins, organs and lesions while projecting them onto its surface. This instructs doctors where veins are located and improves accuracy when inserting a needle, for example. This also enables the detection of tumors and locations of inflammation, thereby providing more precise diagnostic and therapeutic accuracy, helping physicians make more informed decisions without invasive interventions (Solovyova, 2023).

Microsoft's HoloLens, a set of MR smart glasses capable of portraying a world where real and virtual elements appear to coexist, is one of the most notable examples. These smart glasses allow physicians to engage with their surroundings using holograms and to perform a variety of exams and simulations with live statistics to extract relevant data, enabling data-driven decision-making. For example, surgeons can create a detailed 3D digital model of a patient's body part, which they can use to digitally simulate a surgery. Then, visual guidance can be provided to the surgeon via AR during the surgery itself (Palumbo, 2022). Furthermore, VR and AR, supported by a 5G network, can play an important role in the education and training of healthcare professionals who can, in a virtual environment, remotely practice surgical procedures.
ImmersiveTouch, a Chicago-based start-up, developed AR and VR technology that enables surgeons to practice surgical procedures outside of the hospital using VR headsets and 3D scans of patients (Comprehensive Surgical Training Using the Power of Augmented and Virtual Reality, 2023). ImmersiveTouch is a surgical training and exploration simulator that transforms 2D patient data in a 3D digital replica and immerses physicians in a 3D surgery environment with realistic virtual body anatomies and haptic instrument replicates. The majority of surgeons who have used this simulator claim it is just like performing actual surgery (Comprehensive Surgical Training Using the Power of Augmented and Virtual Reality, 2023; Solovyova, 2023).

Surgeries Will No Longer Be Limited to the Operation Room
The physical separation between a surgeon and his patient is not a new concept. In the 1970s, the United States National Aeronautics and Space Administration (NASA) pioneered the idea of remote surgery, or telesurgery, when attempting to treat astronauts in space (Johnson & G, 2016). A decade later, veterinarian Hap Paul and orthopedic surgeon William Bargar created the first surgical robot, the Robodoc (Integrated surgery Systems, Sacramento, CA), an orthopedic image-guided device for hip replacements (Davies 1993; Johnsen 1967; Paul 1992). Robotic surgery enabled surgeons to work with greater precision and accuracy while providing better access to difficult internal body regions (Lanfranco et al., 2004). Telesurgery became a viable option as a result of lightning-fast communication and advances in robotic surgery and equipment (Shahzad et al., 2019). The feasibility and safety of robotic telesurgery was first demonstrated by performing robotic-assisted procedures on pigs in the late 20th century. Six pigs successfully underwent robotic laparoscopic cholecystectomy (removal of the gall bladder) in Strasbourg while the surgeon was in New York, a transatlantic round trip of almost 14,000 kilometres. These surgeries demonstrated that signal transmission latency did not affect surgical performance and that the procedure was safe (Marescaux et al., 2001).
Telesurgery is a branch of medicine that has gained recognition over the past two decades, using wireless networks and robotic technology to allow surgeons to operate on patients remotely. The premise is simple: a highly experienced surgeon performs a surgical procedure on a patient while not present in the operating room. The surgical process is carried out with the assistance of two major pieces of equipment: a robotic one installed in the operating room, known as the ‘slave’, and a remote station from which the surgeon controls the robot, known as the ‘master’ control console. Both systems communicate via a specialized internet connection (Lanfranco et al., 2004; Mohan et al., 2021). In 2001, Professor Jacques Marescaux led a surgical team in New York, USA that successfully performed the world's first transatlantic robotic telesurgery on a human patient in Strasbourg, France (Marescaux, 2001, Korte et al., 2014; Raison et al., 2015). The surgery lasted 54 minutes and was very successful, with the patient recovering without any complications. Dubbed Operation Lindbergh, it represented an important surgical milestone which according to Professor Jacques Marescauxlaid: "lays the foundations for the globalization of surgical procedures, making it possible to imagine that a surgeon could perform an operation on a patient anywhere in the world" (Marescaux, 2001, Korte et al., 2014). Two years later, the first telerobotic remote surgical system was set up in Canada. However, the growth of remote surgery has been challenging since then. While early designs were constrained by primitive computer interfaces, data transmission speed remains a major hurdle in long-distance telesurgery today (Johnson & G, 2016; Mohan et al., 2021). The integration of new technologies, such as fifth-generation (5G) internet is shifting the fate of surgery as it tackles telesurgery’s major challenge of high latency. A delay in conveying auditory, visual, and even tactile information across distant places not only results in a lengthier surgery but also in considerable surgical inaccuracy, which can jeopardize patient safety and retard recovery (Mohan et al., 2021).
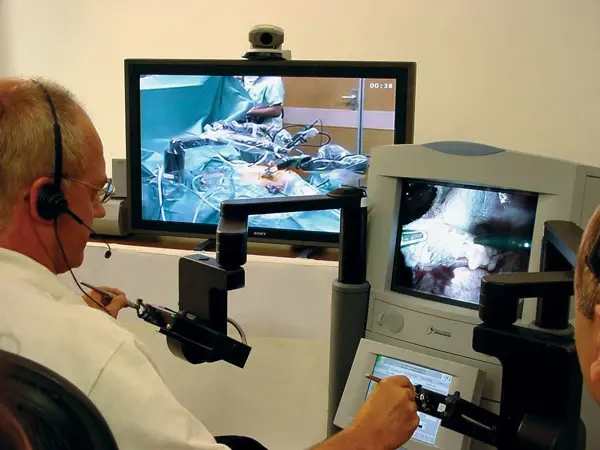
Telesurgery brings many advantages as it allows to overcome current challenges such as a shortage of surgeons, geographical barriers, high financial burden, potential complications, and long-distance travel (Mohan et al., 2021; Satcher et al., 2014). Moreover, telesurgery is a minimally invasive procedure with tinier incisions being made in comparison to traditional surgery techniques. It also opens avenues for international surgical collaboration, connecting specialists from all over the world to review the performance of highly complex surgeries in real time (Mauricio, 2022; Navarro et al., 2022). This technology not only benefits patients, but also improves technical precision and ensures surgeon safety. While telesurgery through robotics is gradually being incorporated into health care practices, this system has become a far-reaching prospect in developing countries due to connectivity difficulties, the demand for expert surgeons at the surgery site, and high expenses (Davis et al., 2016). Nonetheless, the addition of haptic feedback and high-resolution image streaming to support such procedures, as well as the low latency and high-throughput connectivity enabled by 5G, opens the door for surgeons to routinely perform remote surgery on patients anywhere in the world in the near future.
Conclusions
The rollout of 5G cellular service will improve much more than simple phone calls. With higher capacity, 5G connection reduces latency to the point where real-time information can be provided, driving telemedicine and revolutionizing future healthcare. During the COVID-19 pandemic, health workers have swiftly adopted telemedicine methods to maintain social distancing and contain the spread of the virus. Smartphones and upgraded laptop cameras have enabled remote sessions or primary healthcare appointments, making it significantly easier for patients to connect with their doctors. The arrival of 5G will increase the capacity to collect and transmit huge amounts of data in real time. Wearable technology will allow patients to quickly communicate data about their health status with their doctor, reducing response times and allowing doctors to advise and suggest whether hospital or clinic admission is warranted. In hospitals, IoT devices will enable much more regular patient monitoring and reduce the burden on caregivers by allowing them to identify and focus on the patients who need the most attention. While robotic surgery has been used for many years, remote surgery performed by a surgeon in another location is now conceivable. In fact, a surgeon could now manage the entire surgery from start to finish from his facility. Remarkably, the greater bandwidth enabled by 5G will lower the time-lag barrier in device connections, allowing the surgeon to get instant feedback on subsequent surgical steps. As a result, surgeons can perform an operation without being in the same geographic location or time zone. In addition, 5G-enabled tele-mentoring services will allow surgeons to be trained to perform difficult surgeries. It also offers opportunities for international surgical collaboration. While the benefits of telesurgery extend beyond geographic boundaries, the expensive cost of developing and operating a telesurgery system has been a disincentive, yet a reduction in component and service costs is opening the way for its broader implementation.
Bibliographical References
Ahmed Solyman, A. A., & Yahya, K. (2022). Evolution of wireless communication networks: from 1G to 6G and future perspective. International Journal of Electrical and Computer Engineering, 12(4), 3943–3950. https://doi.org/10.11591/ijece.v12i4.pp3943-3950
Attar, H., Issa, H., Ababneh, J., Abbasi, M., Solyman, A. A. A., Khosravi, M., & Said Agieb, R. (2022). 5G System Overview for Ongoing Smart Applications: Structure, Requirements, and Specifications. Computational Intelligence and Neuroscience, 2022, 1–11. https://doi.org/10.1155/2022/2476841
Augmented Reality vs Virtual Reality. (2022). TeamViewer. https://www.teamviewer.com/en/augmented-reality-ar-vs-virtual-reality-vr/
Castro e Melo, J. A. G. de M. e, & Faria Araújo, N. M. (2020). Impact of the Fourth Industrial Revolution on the Health Sector: A Qualitative Study. Healthcare Informatics Research, 26(4), 328–334. https://doi.org/10.4258/hir.2020.26.4.328
Comprehensive Surgical Training using the power of Augmented and Virtual Reality. (2023). Immersive Touch. https://www.immersivetouch.com/immersivesim-training
Corliss, W., & Jhonson, E. (1967). Teleoperators and human augmentation. An AEC-NASA technology survey (Design and application potentials of general purpose, dexterous, cybernetic machines for human augmentation).
Datta, P. (2021). The promise and challenges of the fourth industrial revolution (4IR). Journal of Information Technology Teaching Cases, 204388692110569. https://doi.org/10.1177/20438869211056938
Davies, B., Ng, W., & Hibberd, R. (1993). Prostatic resection: An example of safe robotic surgery. Robotica,11(6), 561-566. doi:10.1017/S026357470001941X
Davis, M. C., Can, D. D., Pindrik, J., Rocque, B. G., & Johnston, J. M. (2016). Virtual Interactive Presence in Global Surgical Education: International Collaboration Through Augmented Reality. World Neurosurgery, 86, 103–111. https://doi.org/10.1016/j.wneu.2015.08.053
Ericsson. (2017). From Healthcare to Homecare: The critical role of 5G in healthcare transformation. Ericsson. (2018). 5G: More than just another ‘G.’ Ericsson, 13. https://www.ericsson.com/assets/local/newsroom/media-kits/5g/doc/ericsson_this-is-5g_pdf_v4.pdf
Haleem, A., Javaid, M., Singh, R. P., & Suman, R. (2021). Telemedicine for healthcare: Capabilities, features, barriers, and applications. Sensors International, 2, 100117. https://doi.org/10.1016/j.sintl.2021.100117
Hardman, J. C., Tikka, T., Paleri, V., Nirmal Kumar, B., Jennings, C., Repanos, C., Stafford, F., Ishii, H., Wheatley, H., Homer, J., Jose, J., McLaren, O., Pracy, P., Simo, R., Sood, S., Lester, S., Winter, S., Kerawala, C., Ah‐See, K., … Yaor, M. (2021). Remote triage incorporating symptom‐based risk stratification for suspected head and neck cancer referrals: A prospective population‐based study. Cancer, 127(22), 4177–4189. https://doi.org/10.1002/cncr.33800
Hatton, M. (2023). The IoT Connectivity Landscape. E271 | Transforma Insights' Matt Hatton. https://www.iotforall.com/podcasts/e271-the-iot-connectivity-landscape
Haverans, R. (2021). From 1G to 5G: A Brief History of the Evolution of Mobile Standards. Brain Bridge.https://www.brainbridge.be/en/blog/1g-5g-brief-history-evolution-mobile-standards
How COVID-19 is changing digital health – and what it means for telcos. (n.d.). STL Partners. https://stlpartners.com/articles/digital-health/how-covid-19-is-changing-digital-health-and-what-it-means-for-telcos/
Hu, H. zhi, Feng, X. bo, Shao, Z. wu, Xie, M., Xu, S., Wu, X. huo, & Ye, Z. wei. (2019). Application and Prospect of Mixed Reality Technology in Medical Field. Current Medical Science, 39(1), 1–6. https://doi.org/10.1007/s11596-019-1992-8
Johnson, B., & G, S. (2016). Robotic Telesurgery: Benefits Beyond Barriers. BMH Medical Journal, 3(2), 51. http://search.ebscohost.com/login.aspx?direct=true&site=eds-live&db=edsdoj&AN=edsdoj.1a1561b4029347c9b9fb556f33ac6780
Korte, C., Sudhakaran Nair, S., Nistor, V., Low, T. P., Doarn, C. R., & Schaffner, G. (2014). Determining the Threshold of Time-Delay for Teleoperation Accuracy and Efficiency in Relation to Telesurgery. Telemedicine and E-Health, 20(12), 1078–1086. https://doi.org/10.1089/tmj.2013.0367
Lanfranco, A. R., Castellanos, A. E., Desai, J. P., & Meyers, W. C. (2004). Robotic Surgery. Annals of Surgery, 239(1), 14–21. https://doi.org/10.1097/01.sla.0000103020.19595.7d
Liu, M., & Ma, Z. (2022). A systematic review of telehealth screening, assessment, and diagnosis of autism spectrum disorder. Child and Adolescent Psychiatry and Mental Health, 16(1), 79. https://doi.org/10.1186/s13034-022-00514-6
Madakam, S., Ramaswamy, R., & Tripathi, S. (2015). Internet of Things (IoT): A Literature Review. Journal of Computer and Communications, 03(05), 164–173. https://doi.org/10.4236/jcc.2015.35021
Makhataeva, Z., & Varol, H. (2020). Augmented Reality for Robotics: A Review. Robotics, 9(2), 21. https://doi.org/10.3390/robotics9020021
Marescaux, J., Leroy, J., Gagner, M., Rubino, F., Mutter, D., Vix, M., Butner, S. E., & Smith, M. K. (2001). Transatlantic robot-assisted telesurgery. Macmillan Magazines Ltd, 413, 379–381. https://pubmed.ncbi.nlm.nih.gov/11574874/
Mauricio, P. (2022). Unleashing the Power of healthcare with 5G. Capgemini Engineering.
Mohan, A., Wara, U. U., Arshad Shaikh, M. T., Rahman, R. M., & Zaidi, Z. A. (2021). Telesurgery and Robotics: An Improved and Efficient Era. Cureus. https://doi.org/10.7759/cureus.14124
Mousavi, S. (2023). Immersive technologies in healthcare - The rise of AR, VR and MR. NHS Arden & GEM. https://www.ardengemcsu.nhs.uk/showcase/blogs/blogs/immersive-technologies-in-healthcare-the-rise-of-ar-vr-and-mr/
Navarro, E. M., Ramos Álvarez, A. N., & Soler Anguiano, F. I. (2022). A new telesurgery generation supported by 5G technology: Benefits and future trends. Procedia Computer Science, 200, 31–38. https://doi.org/10.1016/j.procs.2022.01.202
NS Medical Staff. (2020). FDA approves BioIntelliSense’ BioSticker on-body sensor for scalable remote care. NS Medical Devices. https://www.nsmedicaldevices.com/news/biointellisense-biostickerbody-sensor/
Palumbo, A. (2022). Microsoft HoloLens 2 in Medical and Healthcare Context: State of the Art and Future Prospects. Sensors, 22(20), 7709. https://doi.org/10.3390/s22207709
Paul, H. A., Bargar, W. L., Mittlestadt, B., Musits, B., Taylor, R. H., Lzanzides, P., Zuhars, J., Williamson, B., & Hanson, W. (1992). Development of a Surgical Robot for Cementless Total Hip Arthroplasty. Clinical Orthopaedics and Related Research, 285, 57???66. https://doi.org/10.1097/00003086-199212000-00010
Raison, N., Khan, M. S., & Challacombe, B. (2015). Telemedicine in Surgery: What are the Opportunities and Hurdles to Realising the Potential? Current Urology Reports, 16(7), 43. https://doi.org/10.1007/s11934-015-0522-x
Satcher, R. L., Bogler, O., Hyle, L., Lee, A., Simmons, A., Williams, R., Hawk, E., Matin, S., & Brewster, A. M. (2014). Telemedicine and telesurgery in cancer care: Inaugural conference at MD Anderson Cancer Center. Journal of Surgical Oncology, 110(4), 353–359. https://doi.org/10.1002/jso.23652
Schwab, K. (2017). The Fourth Industrial Revolution (1st ed.). Crown Business.
Shahzad, N., Chawla, T., & Gala, T. (2019). Telesurgery prospects in delivering healthcare in remote areas. JPMA. The Journal of the Pakistan Medical Association, 69 1)(1), S69–S71. https://pubmed.ncbi.nlm.nih.gov/30697023/
Solovyova, V. (2023). AR & VR In Healthcare: 4 Use Cases with Real-Life Examples. Softeq.
The Digital Advantage: What is the Future of Business? (2019). Maxis. https://www.business.maxis.com.my/en/spark/insights/the-digital-advantage-what-is-the-future-of-business/
Vodovatova, E. (2023). Augmented and virtual reality in medicine and health care. The App Solutions. https://theappsolutions.com/blog/development/ar-vr-in-healthcare/
Walker, R., Hillhouse, M., Perrochet, B., Sparenborg, S., Mooney, L., & Ling, W. (2019). Medication Adherence Monitoring Using Smartphone Video Dosing in an Open-label Pilot Study of Monthly Naltrexone Plus Once-daily Bupropion for Methamphetamine Use Disorder: Feasibility and Acceptability. Journal of Addiction Medicine, 13(5), 372–378. https://doi.org/10.1097/ADM.0000000000000509
Whelan, K. (2022). 5G-Connected Ambulances Revolutionize Emergency Care. E-Magazine by Medical Expo. https://emag.medicalexpo.com/smart-ambulances-revolutionize-emergency-care/#:~:text=Technology is revolutionizing emergency care,advanced augmented%2Fvirtual reality support.
Xushenglan. (2021). Transforming Healthcare with 5G. Huawey. https://www.huawei.com/en/huaweitech/publication/winwin/38/transforming-healthcare-5g
Yang, Y., Yuan, Y., Zhang, G., Wang, H., Chen, Y.-C., Liu, Y., Tarolli, C. G., Crepeau, D., Bukartyk, J., Junna, M. R., Videnovic, A., Ellis, T. D., Lipford, M. C., Dorsey, R., & Katabi, D. (2022). Artificial intelligence-enabled detection and assessment of Parkinson’s disease using nocturnal breathing signals. Nature Medicine, 28(10), 2207–2215. https://doi.org/10.1038/s41591-022-01932-x
Visual Sources
Figure 1 - O’Dowd, E. (2017). 5G Network Infrastructure Improves Telemedicine, Remote Care. Hit Infrastructure. [image]. https://hitinfrastructure.com/news/5g-network-infrastructure-improves-telemedicine-remote-care
Figure 2 - Ross, C. (2020). Hospitals turn to remote monitoring tools to free up beds for the sickest coronavirus patients. STAT. https://www.statnews.com/2020/03/25/coronavirus-hospitals-weigh-remote-patient-monitoring-tools/
Figure 3 - Whelan, K. (2022). 5G-Connected Ambulances Revolutionize Emergency Care. E-Magazine by Medical Expo. https://emag.medicalexpo.com/smart-ambulances-revolutionize-emergency-care/#:~:text=Technology is revolutionizing emergency care,advanced augmented%2Fvirtual reality support.
Figure 4 - Jha, G., Sharma, L., & Gupta, S. (2021). E-health in Internet of Things (IoT) in Real-Time Scenario. In Lecture Notes in Networks and Systems: Vol. 203 LNNS. [image]. https://doi.org/10.1007/978-981-16-0733-2_48
Figure 5 - ImmersiveTouch Inc. (2023). A case of how surgical planning in 3D is better than 2D. Facebook. [image]. https://www.facebook.com/immersivetouch/posts/pfbid02PMZMHJVYHYprN7aDi7AETwmoyWM5Z1uf45654EssCeURGPaUmqHdM5o74AR569RHl?__tn__=%2CO*F
Figure 6 - Marescaux, J., Leroy, J., Gagner, M., Rubino, F., Mutter, D., Vix, M., Butner, S. E., & Smith, M. K. (2001). Transatlantic robot-assisted telesurgery. Nature, 413(6854), 379–380. https://doi.org/10.1038/35096636




Leveraging 5G for robotic telesurgery holds immense potential for revolutionizing healthcare. With ultra-low latency and high-speed data transmission, 5G enables surgeons to operate robotic systems remotely with precision and real-time feedback. This could greatly enhance access to specialized care in underserved areas. However, reliable 5G networks are essential, and some users have expressed concerns about service quality. For more information on customer feedback, check verizon phone number. Ultimately, 5G will be instrumental in making telesurgery more efficient, safer, and accessible worldwide.
thanks a lot for information! The Attract Group's study offers an in-depth look at the on-demand app industry, providing valuable insights and trends. Their analysis is both comprehensive and accessible, making it an essential read for entrepreneurs and businesses looking to venture into the on-demand economy or refine their existing services.